Clean claims are those that have left the healthcare organization, successfully passed the clearinghouse claims editor and have been accepted by the payer without additional human intervention. Simply put, clean claims are paid the first time without any additional intervention. Because this result is so coveted, revenue cycle leaders closely monitor their clean claims rates, and they aspire to a perfect 100% of clean claims. While this is a lofty goal, most revenue cycle management (RCM) experts believe organizations with a 95 – 97% clean claims rate are high performing.
Why is being paid the first time so important? Because when claims are rejected or denied, more than half of them run the risk of never being paid, says the Medical Group Management Association (MGMA). And it takes time to analyze the reason the claim was rejected and remedy the issue before the healthcare organization can resubmit it.
Industry averages show 20% of all healthcare claims are denied. Becker’s Hospital CFO Report says 10% of all hospital claims are denied or rejected, adding up to $5 million per year for the average hospital.
Denied claims not only delay payment of the claim, but your organization must also spend additional money to fix and resubmit the claim in hopes of getting paid. Sometimes this is merely throwing good money after bad. That is why so much focus is spent preventing the denial in the first place.
Add to that, denied claims are becoming increasingly common. A recent MGMA study found that 69% of healthcare organizations reported denials have increased, while medical groups reported an increase of 17%.
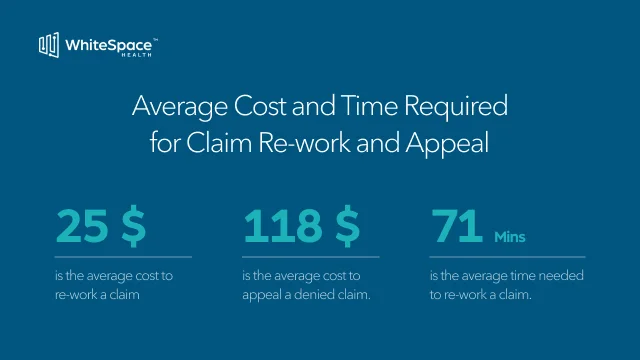
An estimated two-thirds of all denied claims are recoverable. Studies estimate the cost to rework a claim at $25. And the administrative cost to appeal a claim can run over $118 each. As a result, many practices and other healthcare organizations simply forgo appealing smaller claims.
Inefficient processes across the revenue cycle collectively cost healthcare organizations billions of dollars each year, says the Council for Affordable Quality Healthcare (CAQH). In 2020, the U.S. healthcare system could have saved $16.3 billion, or 42% of the $39 billion spent on administrative transactions, says the CAQH Index.
Staffing figures prominently in the cost of filing claims and chasing denials, but revenue cycle management (RCM) staff is increasingly harder to come by in the post-pandemic job market. This is especially true for the critical leadership roles.
Health systems and medical groups rely primarily on experienced leaders to pass on the nuances of filing clean claims by word of mouth and on-the-job training. Few organizations maintain written or electronic standard operating procedures (SOPs).
Even in the best of circumstances, with the right staff and a standard operational procedure (SOP), it can take new staff years to come up to speed with the complex workstreams, government guidelines and payer nuances. Quarter changes in coding and payer guidelines, semi-annual updates to CPT and ICD coding schemas not to mention constant updates to technology, policy and organizations all combine to create an environment that is always changing. One small change in any one of these areas could result in a rejected or denied claim – and added cost to getting paid.
The answer to the overwhelming pressure of denied claims is artificial intelligence (AI). In short, our ever-learning capabilities recommend actions that have resolved similar issues in the past. Knowing what historical steps have been successful is essential to staying ahead of so much constant change and at such granular levels.
WhiteSpace offers AI-powered solutions can detect, predict, and resolve RCM issues. Our robust business intelligence solution combines advanced technology, including ever learning, predictive analytics, data services, and a health data warehouse to transform your data into hard dollar financial improvements.
- Prior authorization was not obtained prior to care.
- Missing or incorrect information on the claim.
- Medical necessity requirements were not met.
- The procedure was not covered by the payer.
- The provider was out of network.
- There were duplicate claims.
- The claim exceeded the timely filing limit.
Our predictive capabilities let you know what has worked previously to create clean claims, what to do when claims need to be re-worked, and what has helped you and other organizations like yours get paid in the past.
This level of data analytics is not possible for even the most seasoned billing professionals to maintain in their heads, or even in a SOP. That is because payer and billing information changes on a daily basis. AI can keep up and notices patterns in your data because it is always learning.
In their battle to prevent denials, many healthcare CBOs struggle with how to prioritize use of their limited resources. WhiteSpace Health’s new solution, Resolution Insight, stretches and adds to your resources by becoming your digital playbook. It is a digital clone created for your RCM process with the ability to manage critical decisions across your central billing office (CBO).
RCM managers know that management of denied claims is more urgent than ever before. Fifty-one percent of the respondents in a recent Part B News survey say they will be “more aggressive” in challenging denied claims in 2023.
But this is not the whole picture. Appeals are done as a last resort, and reclaiming the money is much more costly and even unlikely in some cases. The best way forward is to keep claims clean in the first place—to proactively bill for money earned. And for that, you need the power of AI. Call us at WhiteSpace Health to learn more about how we can help manage your denials and boost your bottom line.
- Provides a digital playbook encompassing all your SOP and best practices.
- Predicts resolution trends and prescribe insights to resolve issues.
- Manages the investigative work needed to take the best courses of correction.
- Recommends how to work the denied or open claims.
- Prioritizes and assign inventory to users.
- Tags and tracks performance.
- Provides specific analytics on actionable and expected reimbursement.
- Manages recurring issues with predictive and prescriptive insights.
About Gautam Char
Gautam Char is the president and CEO of WhiteSpace Health. He has a wealth of experience bringing products to market and rapidly growing companies. Known for building high performance teams that create valuable products and solutions for customers, Char’s talent for collaboration and his industry knowledge will position WhiteSpace Health for growth and excellence.